Introduction
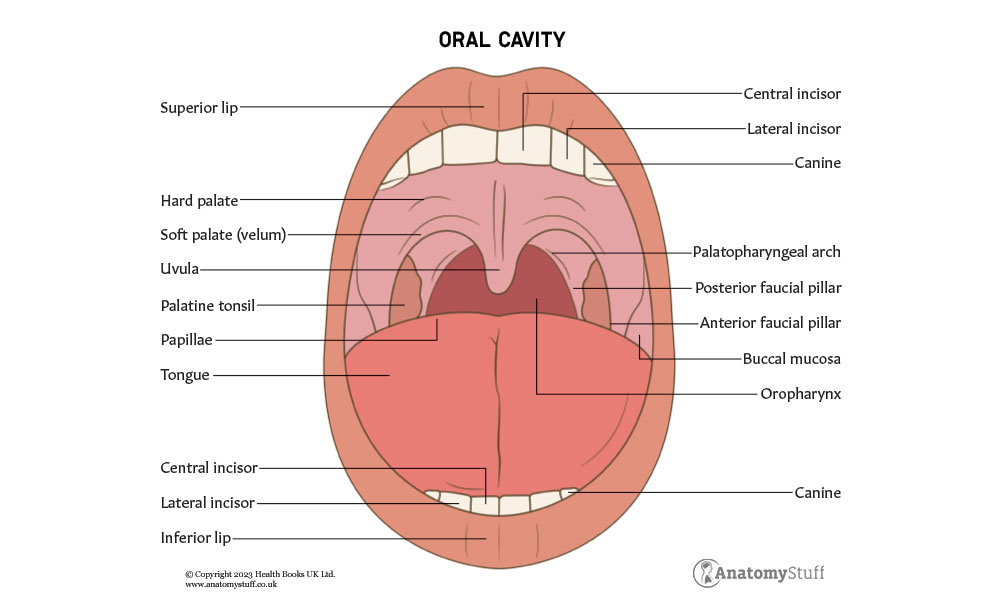
The tongue is a muscular organ found within the oral cavity. It plays an integral role in many life-sustaining processes, such as taste, mastication (chewing), swallowing and speaking. It is covered by oral mucosa and contains intrinsic and extrinsic muscles. Keep reading to discover all about the intricate anatomy of the tongue as well as relevant conditions such as oral candidiasis (thrush) and Kawasaki Disease (a type of vasculitis).
Function
The tongue functions as a digestive organ. As mentioned above, it facilitates the movement of food during mastication and swallowing as well as aiding with taste and speech.
Fun fact: In Latin, the tongue is called ‘lingua’. Knowing this will help you remember the blood supply to the tongue – via the lingual artery and vein. Also, in Greek, the tongue is called ‘glóssa’, and both the hypoglossal and glossopharyngeal nerves play a major role in motor and sensory innervation.
Anatomy
The human tongue can be divided into the anterior 2/3 and the posterior 1/3. The anterior 2/3 comprises part of the oral cavity, whereas the posterior 1/3 is considered part of the oropharynx. This division is important when learning about the sensory innervation of the tongue (discussed in more detail below).
The tongue is also separated medially by a structure called the lingual septum.
Location
The root of the tongue is connected to the hyoid bone via the hyoglossus and genioglossus muscles, a U-shaped bone in the anterior compartment of the neck. The tongue occupies the floor of the oral cavity, and the apex makes contact with the teeth.
Muscles
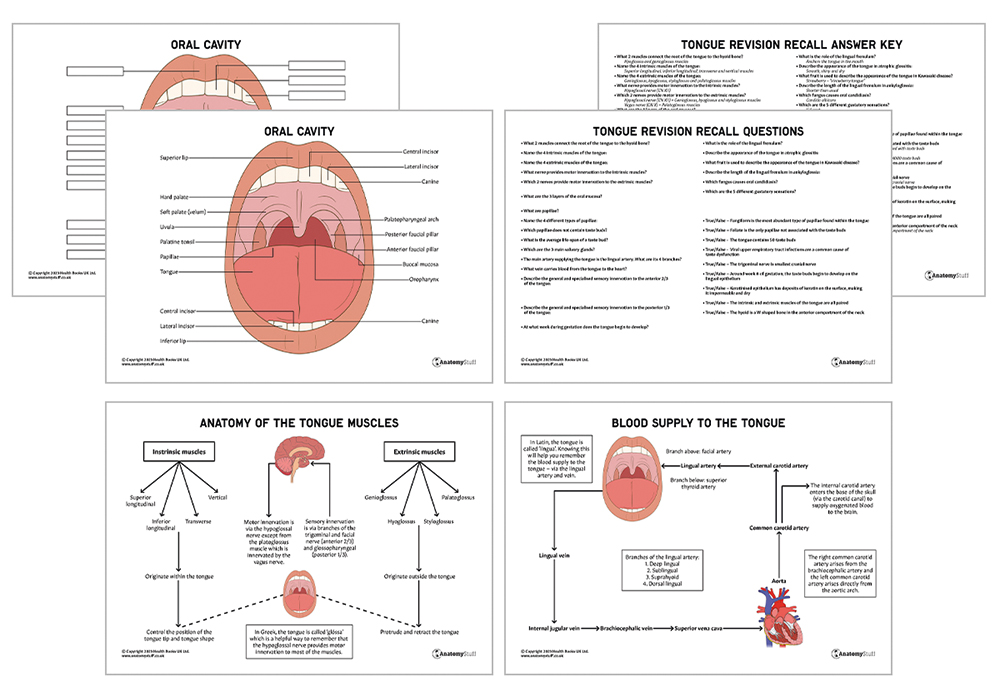
The tongue is formed from 8 paired muscles that can be divided into 2 groups: intrinsic and extrinsic muscles. These muscles allow the tongue to change shape and position. They are all innervated by the hypoglossal nerve (CN XII) except the palatoglossus muscle.
| Type of muscle | Name of muscle | Innervation |
| Intrinsic | Superior longitudinal | CN XII |
| Inferior longitudinal | CN XII | |
| Transverse | CN XII | |
| Vertical | CN XII | |
| Extrinsic | Genioglossus | CN XII |
| Hyoglossus | CN XII | |
| Styloglossus | CN XII | |
| Palatoglossus | CN X (vagus nerve) |
The four extrinsic muscles arise from outside the tongue, whereas the intrinsic muscles originate and insert within the tongue. The intrinsic muscles are not attached to any bones.
Although both muscle groups work very closely together, it is thought that the extrinsic tongue muscles primarily protrude and retract the tongue, and intrinsic muscles control the position of the tongue tip and tongue shape.
Microscopic anatomy
Oral mucosa: within the oral cavity, a mucous membrane called the oral mucosa lines the structures. It is formed by three layers (order from superficial to deep):
• Surface squamous stratified epithelium (also known as oral epithelium)
• Lamina propria (connective tissue)
• Submucosa (not present in all regions)
Based on their function, various areas of the oral cavity contain different types of oral mucosa, either keratinised oral mucosa or non-keratinised oral mucosa.
Papillae: small, raised protrusions on the dorsal tongue that contain the taste buds. There are four different types of papillae:
• Circumvallate (or vallate)
• Fungiform
• Filiform (most abundant)
• Foliate
All except the filiform papillae are associated with taste buds.
Refresher
Keratinised epithelium has deposits of keratin on its surface. This makes it impermeable and dry. Examples of where this type of epithelium can be found within the body include the skin and sole of the foot.
On the other hand, stratified squamous epithelial cells lack the keratin protein. Therefore, they are called non-keratinised epithelium. This type of epithelium can be found in the lips, upper oesophagus, conjunctiva of eyes, rectum, vagina and more.
Taste buds
The tongue contains approximately 2000-4000 taste buds situated within the small structures known as papillae (discussed above) found on the tongue’s upper surface, soft palate, upper oesophagus, cheek, and epiglottis.
These microscopic sensory organs are responsible for the perception of five different gustatory sensations: sweet, salty, sour, bitter, and umami (a Japanese word meaning “pleasant savoury taste” and has been described as brothy or meaty). Each type of taste bud is able to detect all five flavours, although some types are more sensitive to certain tastes.
They convert taste stimuli into electrical signals, which are then transferred to the sensory nerves and sent to the brain. They have an average life span of 8-12 days, although some do remain for much longer.
Taste dysfunction is a relatively common presentation amongst patients and can cause serious consequences like anorexia and malnutrition. Viral upper respiratory tract infections are common causes.
Saliva
Not only is saliva necessary for the perception of taste, but taste is an important stimulus for saliva production. Saliva is made, modified and secreted from the salivary glands. These three paired glands (parotid, submandibular, and sublingual) contribute to approximately 90% of the human body’s saliva secretions. The remaining 10% of saliva secretions are made, modified and secreted from minor salivary glands.
Blood supply
The main artery supplying the tongue is the lingual artery. This is a major branch of the external carotid artery and arises from the external carotid artery between the superior thyroid artery and the facial artery.
The lingual artery has 4 branches:
1. Deep lingual
2. Sublingual
3. Suprahyoid
4. Dorsal lingual
Venous drainage of the tongue is via the lingual vein.
Refresher
The external carotid artery is one of the two terminal branches of the common carotid artery. It supplies areas of the head and neck external to the cranium. The other branch, the internal carotid artery, enters the base of the skull (via the carotid canal) to supply oxygenated blood to the brain.
Innervation
As discussed above, the hypoglossal nerve provides motor innervation to all muscles, intrinsic and extrinsic. The only exception is the palatoglossus muscle which is innervated by the vagus nerve.
In order to understand all about sensory innervation to the tongue, it is necessary to split the tongue into the anterior 2/3 and posterior 1/3 as well as dividing the types of sensory innervation:
• General sensory stimulation: most organs in the human body can detect general sensory stimulation, specifically temperature, touch and pain.
• Specialised sensory innervation: specialised organs such as the tongue or the nose (which play a role in taste and smell) contain specialist sensory innervation.
Nerves supplying the general and specialised sensory innervation of the tongue:
• Sensory sensation to anterior 2/3 = Branch of the trigeminal nerve (CNV). Specifically, the lingual nerve, which is a branch of the mandibular nerve (CN V3).
• Gustatory sensation in the anterior 2/3 = Branch of the facial nerve (CN VII), specifically the chorda tympani.
In the posterior 1/3 of the tongue, both general sensory and specialised (taste) innervation is supplied by the glossopharyngeal nerve (CN IX).
Refresher
The trigeminal nerve is the fifth and largest cranial nerve (CN V). It provides sensory innervation to the skin, mucous membranes and sinuses of the face. It has three main branches:
• Ophthalmic (V1)
• Maxillary (V2)
• Mandibular (V3)
Embryology
The tongue begins to develop around the 4th week of gestation. It arises from the pharyngeal arches. Around week 8 of gestation, the taste buds begin to develop on the lingual epithelium.
Interestingly, as the tongue initially forms, it is tethered to the floor of the oral cavity. However, a process called sculpting apoptosis releases the tongue and leaves behind a structure called the lingual frenulum, which anchors the tongue in the mouth.
Clinical relevance
Many medical conditions can have oral manifestations; therefore, it is always important to examine the tongue as part of a clinical examination. Also, understanding some of these conditions will help make the anatomy a lot easier to remember!
Atrophic glossitis = The partial or total absence of filiform papillae on the dorsal surface of the tongue. The tongue might also look smooth, shiny and dry.
Kawasaki disease = A common type of paediatric vasculitis (inflammation of blood vessels) which can present as a ‘strawberry tongue’ (as well as fever, rash and heart problems). The tongue looks this way due to inflamed and hypertrophic fungiform papillae and hyperemia (increased amount of blood in the blood vessels of an organ or tissue in the body).
Ankyloglossia (tongue-tied) = Occurs when the lingual frenulum (a thin strip of anchoring the tongue to the floor of the mouth) is shorter than usual. This is usually diagnosed during a newborn physical examination and can be cut with sterile scissors by a healthcare professional if necessary.
Oral candidiasis = A fungal infection involving the accumulation of Candida albicans within the mouth. White patches can develop over the tongue and can be linked to medication such as inhaled corticosteroid use (for example, in an asthmatic patient).
Additionally, many different nutritional deficiencies can lead to oral manifestations, particularly with signs directly on the tongue. For example, vitamin B6 deficiency can lead to a sore tongue and iron deficiency can cause the tongue to become painful and burn. Hence, examining the tongue and asking about any associated symptoms during consultations with patients is very important.
Related Products
View All